When it comes to health plans, provider network adequacy is crucial. For most health insurance products, it is mandated by law that health insurers ensure that their networks are sufficient in size and scope to offer a defined set of covered services to their members. However, provider network adequacy does not always equate to actual member access.
Fact or Myth?
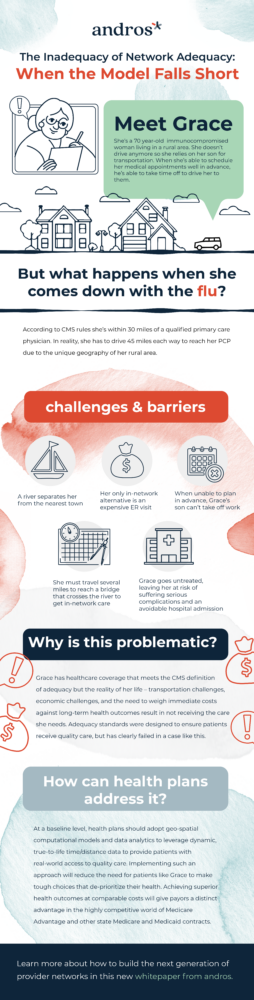
It is important to note that just because a provider network is deemed adequate, it does not necessarily mean that members have easy access to healthcare services. In fact, there are several factors that can affect member access even within an adequate provider network.
One of the major factors is the availability of providers. Even if a health plan has sufficient numbers of providers in a particular area, if those providers are not accepting new patients or have long wait times, then members may still face difficulty accessing care. Additionally, the sub-specialties of providers within a network can also impact member access. Providers who lack experience or knowledge in a certain area may not be able to provide the level of care that members need and this can lead to decreased access.
Another major issue related to provider network adequacy is the issue of distance. A network may be deemed adequate, but if the providers within that network are spread out over long distances, or inaccessible via public transportation, then members may still face significant barriers to care. This is particularly a concern in rural areas where long distances and lack of accessibility can pose significant challenges for members seeking medical care.
Network adequacy should not only be viewed as a matter of geography or numbers of providers either. Health plans must also consider the cultural and linguistic needs of their members. Providers who are unable to communicate with their patients are less likely to be effective in providing adequate care. Cultural barriers, such as lack of understanding of certain norms and traditions, can also lead to lower access.
In addition, members with certain health conditions may require specialized care that is only available within a certain network. Health plans should consider specialized needs when developing a provider network that is adequate for their members. For example, medicall children with complex medical needs or requiring long term support and services require home and community based services from providers with experience serving the pediatric population.
Be More Than Adequate
The misconception that achieving “provider network adequacy” equals member access to care is a dangerous one. Health plans and organizations must not only ensure that their networks are sufficient in size and scope but also consider the factors that can seriously limit members’ access to care. Factors such as the availability and quality of providers, the availability of specialized care, distance, culture, and language all play crucial roles in determining whether members can easily and effectively access healthcare services. Health plans and organizations must address these challenges and actively work to ensure that their members have true access to healthcare services. The promise of adequate provider networks must extend beyond just numbers and geography to truly change lives for the better.
Let’s be more than adequate together!