CMS introduced the Global and Professional Direct Contracting (GPDC) Model in 2020 to build on previous successes and continue transforming the world of value-based care. What does the new program entail and how can participants maximize their opportunities to succeed?
A decade after the launch of the first accountable care organizations (ACOs), the healthcare industry has come a long way—but it still has a lot to learn about value-based care.
The early days of payment transformation were marked by both encouraging successes and high-profile failures as regulators, providers, and payers experimented with different ways of working together to boost outcomes, reduce costs, and improve experiences.
While the learning process has been frustrating at times, there’s no denying the fact that value-based care can be effective if implemented correctly.
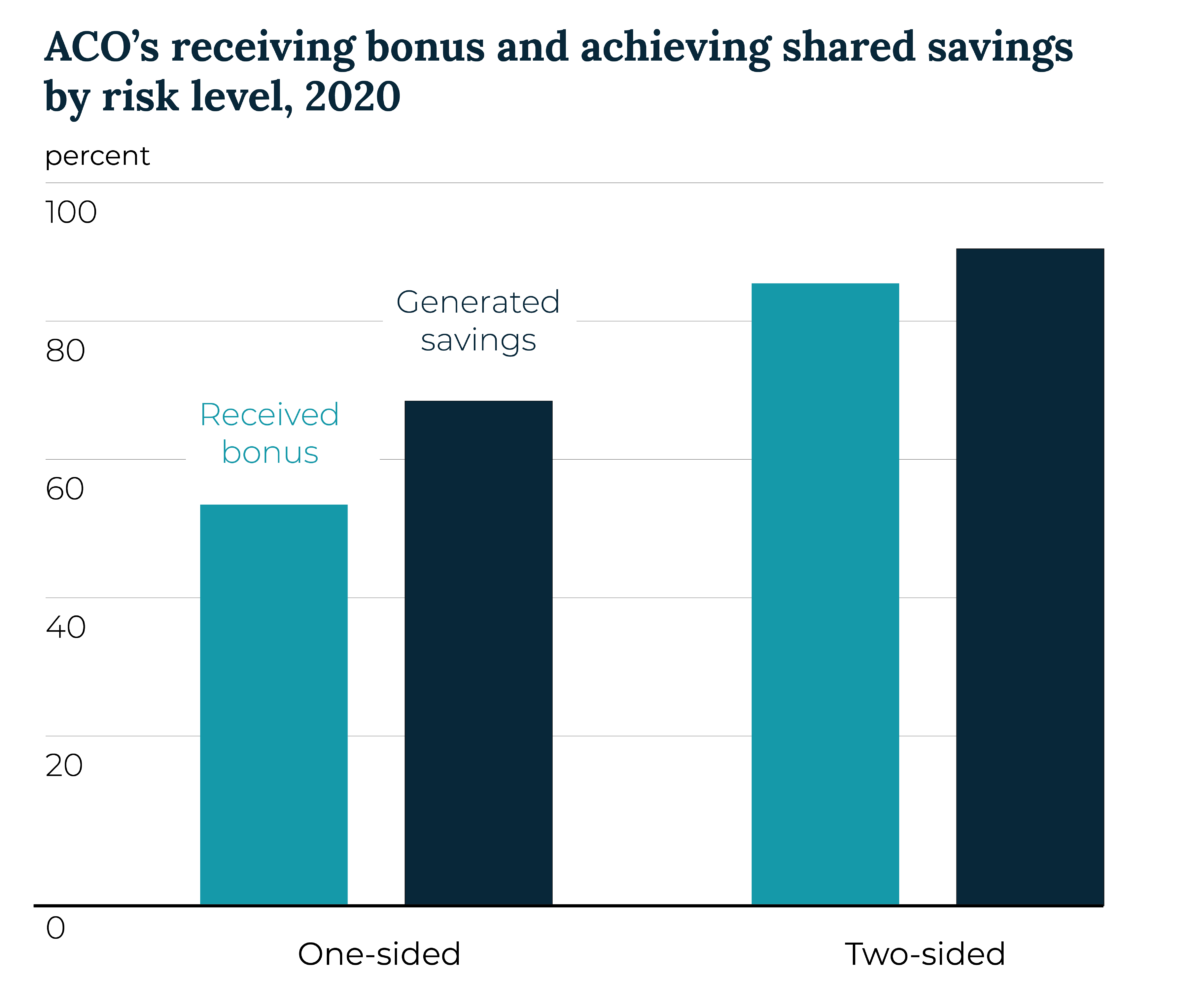
Even amidst the uncertainty and stress of the COVID-19 pandemic, for example, ACOs in the Medicare Pathways to Success program generated average net savings of $190 per beneficiary – nearly twice the rate of the 2019 performance year – and 67 percent of ACOs earned shared savings bonuses. These positive financial outcomes are a direct result of improvements to care quality, illustrating the importance of aligning incentives to encourage holistic, proactive patient care.
But the Centers for Medicare and Medicaid Services (CMS) isn’t done yet. The agency is continuing to develop its value-based care programs to further enhance its accomplishments while eliminating some of the pain points of past initiatives.
The Global and Professional Direct Contracting (GPDC) Model is the latest iteration of value-based care, designed to test a variety of risk-sharing arrangements for providers serving traditional Medicare fee-for-service populations.
With a focus on leveraging primary care to produce better outcomes, GPDC offers innovative risk-sharing options suitable for both experienced providers and those new to the pay-for-performance environment.
There are similarities to existing ACO programs, including the use of Direct Contracting Entities (DCEs) that function as the administrative link between CMS and groups of provider participants. But GPDC differs somewhat in its financial structure, offering higher risk levels and higher rewards to motivate and empower primary care providers and their partners across the care continuum.
Participants in GPDC will need to develop strong communities of quality providers that are willing and able to succeed on the cutting edge of value-based care. Doing so will require an agile, proactive, data-driven recruitment strategy and the ability to monitor ongoing performance over the course of the model’s lifetime.
Exploring the basics of the Global and Professional Direct Contracting Model
From its introduction in 2020, CMS has positioned GPDC as a direct successor to its ever-evolving lineup of accountable care options.
“The Direct Contracting Model leverages lessons learned from other Medicare ACO initiatives, such as the Medicare Shared Savings Program and the Next Generation ACO (NGACO) Model, as well as innovative approaches from Medicare Advantage (MA) and private sector risk-sharing arrangements … to use the redesign of primary care as a platform to drive broader health care delivery system reform,” the agency stated in its guidance to the industry.
GPDC intends to accomplish this goal by reducing administrative complexity, focusing more on outcomes metrics for quality measurement, allowing providers to offer enhanced benefits to patients, and emphasizing voluntary patient attribution instead of relying solely on a preponderance of claims.
CMS anticipates that GPDC will create more predictable and prospective spending targets that adequately account for the challenges of working with complex and chronically ill populations.
The driving force behind the model is the requirement to shoulder significant financial accountability. Currently, participants can choose from two separate pathways with different levels of risk and reward:
Professional: This lower risk option offers 50 percent shared savings and shared losses, subject to risk corridors. There is also an element of capitation for primary care services. The Primary Care Capitation (PCC) structure is a risk-adjusted monthly payment for primary care services and will typically equal 7 percent of the performance year benchmark.
Global: The global category includes 100 percent savings and losses paid either through the PCC method or through Total Care Capitation (TCC), which is a risk-adjusted monthly payment for all covered services.
CMS is also considering a third option to assume total cost of care risk for Medicare Parts A and B in a defined geographical target region, but that branch of the program is under review and will not be available by the start of the next performance year on January 1, 2022.
The federal agency hopes to attract a wide variety of provider types interested in taking up the challenge, including existing ACO groups, independent provider associations (IPAs), hospital systems, integrated delivery networks, Medicaid Managed Care Organizations (MCOs), and even skilled nursing facilities.
Looser affiliations of hospital and physician practices are also welcome to join, and providers do not need to have any previous experience with value-based reimbursement in order to take part in the program.
Participant groups will form Direct Contracting Entities (DCEs) that fall into one of the three following categories:
Standard DCEs: The Standard DCE is for providers with extensive experience serving Medicare fee-for-service (FFS) populations. They may also serve dual-eligible Medicare/Medicaid beneficiaries. Because they have existing Medicare FFS beneficiaries, attribution will rely on a mix of voluntary and claims-based alignment. Entities may or may not have participated in previous value-based care models, such as the Next Generation ACO, Pioneer ACO program, or Pathways to Success, and may have varying levels of risk tolerance.

New Entrant DCEs: New entrants are providers who have not served a large number of Medicare FFS beneficiaries in the past. Initially, attribution may be conducted on a voluntary basis, although claims-based alignment will also be used to develop a patient panel.

High Needs Populations DCEs: These DCEs will include providers who serve Medicare FFS with complex needs. Providers in this category will be expected to use evidence-based care models designed for high-needs individuals.
CMS is reviewing a fourth category, as well, which would be specifically geared to MCOs who manage dual-eligible populations.
The timeline for GPDC is somewhat unique, consisting of an implementation period (which took place in 2020), an initial performance period from April 2021 to December 2021, and a further five full years of performance measurement aligned to the calendar year.
While the initiative has already begun, the participation list isn’t set in stone. Existing and newly licensed DCEs have the opportunity to continue recruiting providers throughout the course of the program to bolster the volume of their attributed patients and ensure the delivery of quality care.
With significant financial incentives on the table, competition to enroll top-performing primary care providers will be fierce. DCEs must carefully strategize to be the first to secure high-value partners with an ideal blend of beneficiaries.
Successfully outmaneuvering competitors will depend on access to accurate, detailed performance data, shrewd negotiation skills, and a thorough understanding of constantly shifting market dynamics.
Building a sustainable, successful DCE to deliver exceptional quality care
As this new value-based care model takes shape, DCEs will need to build a network of primary care partners that is fully equipped to take on the challenges of the program’s ambitious risk structure.
With so much on the line, DCE leaders will have to carefully assess potential provider partners for their suitability across a variety of domains, including their patient panel size, appetite for financial risk, and capacity for clinical transformation.

Establishing guidelines for the right clinical and cultural fit
DCEs are voluntary associations of providers, so leaders have some leeway in choosing who they wish to include in their network.
Defining the criteria for membership will depend, first of all, on the chosen DCE category. New Entrant DCEs will need to specifically seek out Medicare novices who anticipate serving an appropriately large number of eligible beneficiaries. This may include newly established physician practices or those who have recently decided to accept Medicare.
Meanwhile, Standard DCEs have more decisions to make. Will the DCE focus on providers who have previous experience with value-based care or recruit providers who are brand new to the pay-for-performance ecosystem?
If the former, is the DCE aiming to work with providers who have achieved shared savings in the past and are eager for more, or will the organization act as an alternative for those who have been frustrated by failure in previous value-based arrangements?
No matter what the positioning, the DCE must ensure that its members have the ability to meet GPDC’s clinical and financial goals.
In all cases, providers will need to demonstrate the ability to deliver proactive, comprehensive care to their patients. A holistic, well-established chronic care management program, along with robust information sharing capabilities, will be key to success on this front.
Prospective participants should also understand how to use appropriate risk adjustment to accurately reflect the clinical challenges of their Medicare populations. They should have processes in place to identify gaps in care and strong relationships with specialists and community-based organizations to close those gaps when necessary.
Providers that have the infrastructure to share the right information with the right people to get the right outcomes for their patients will likely be highly sought after by multiple DCEs.
That means DCEs will also have to make themselves attractive to their top targets by showcasing their strategic plan and any technical, financial, clinical, or policy support available to members throughout the course of the participation period.
Finding the optimal mix of performance and patient panel size
Just like accountable care organizations, DCEs have the ability to change their composition and grow over time. Entities will be looking for two major factors when plotting out their recruitment strategies: clinical performance and patient panel size.
DCEs will need to feel comfortable that their member providers are delivering care that results in high marks on quality measures, positive outcomes for beneficiaries, and spending rates that fall within the benchmarks of their chosen reimbursement model.
They also need to focus on scale. Standard DCEs will need to enter the program with a minimum of 5000 aligned Medicare beneficiaries. New Entrant DCEs have several years to build up to 5000 lives but must start with at least 1000 patients.
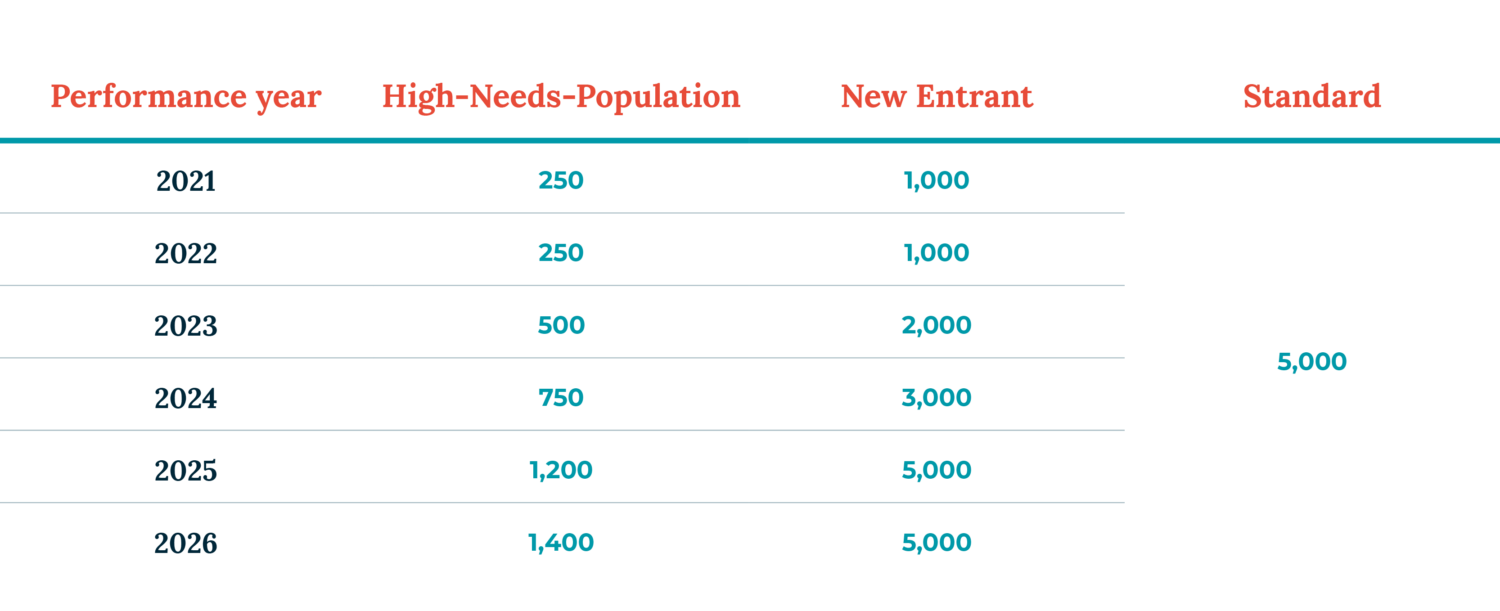
However, there will be several benefits to exceeding these minimums. For example, a larger pool of beneficiaries may mean more healthy individuals to balance out the 10 percent of patients that account for nearly half of Medicare spending, which is critically important in capitation structures.
But DCEs will not have unlimited resources to secure involvement from these high-performing providers and ideal patient groups. Most cannot afford to go through lengthy recruitment and contracting processes with hundreds of disparate partners only to gain a few thousand covered lives. A fragmented network is likely to be more difficult to administer and will be at a greater risk of failure due to poor communication and competitive market forces.
That may leave some DCEs with an incentive to focus on large provider groups that can help them achieve scale with fewer conversations and less effort. These larger groups may also already have access to the technical infrastructure and staffing resources required to do well in pay-for-performance models, improving the likelihood of speedy success.
That doesn’t mean smaller providers will be relegated to the fringes of the next wave of value-based care. With its reduced administrative complexity and flexible risk sharing options, the GPDC program is designed to make it easier for rural physicians, Federally Qualified Health Centers (FQHCs), and others to launch DCEs with their specific goals in mind.
Many of these specialized groups are likely to prioritize quality over scale. If they focus on establishing accurate risk adjustment processes for their populations, the chances of financial success are just as good as with larger entities.
Leveraging data to efficiently to recruit and retain high-value providers
With goals in mind and provider types targeted, DCEs will move on to choosing specific primary care practices to reach out to. They will need a mechanism to identify candidates that meet their criteria, deliver education about GPDC to those organizations, and tailor their pitch to the unique factors that are most important to those clinicians.
Data will be crucial for completing this process efficiently and effectively. DCEs will need access to detailed market information, such as provider size and location, information on clinical performance, previous value-based care participation, existing business affiliations, and claims volume.

Because DCEs can operate in multiple, non-contiguous geographic regions, it may be challenging for entities to compile all this information on their own. Therefore, DCEs should consider working with a partner of their own on this process. By collaborating with a clinical network development expert that provides similar services to local and national health plans, DCEs can gain advantageous insights into the territories and provider groups that are of the most interest to them.
With a thorough understanding of the provider landscape, DCEs can establish a core network of primary care providers while leveraging those relationships to access to the high-performing specialists and ancillary providers that create effective communities of care.
Enlisting help with the recruitment process can also stretch scarce resources further. DCEs may not have the staff to conduct outreach at the pace required to reach out to an entire list of providers, follow up as many times as necessary, and answer preliminary questions about the program and its benefits.
Speed and efficiency will be of the essence as other first generation DCEs try to woo the same set of interested primary care providers. And should the program expand in future years, even more competitors are likely to be wrestling over the loyalty of a finite number of physician practices. Getting ahead of the game now with rich, actionable data and outreach capabilities will serve these foundational DCEs well in years to come.
Looking forward to the future of value-based care
The Global and Professional Direct Contracting model is intended to build upon the momentum of value-based care and gauge the industry’s interest and ability to take on capitation in the modern reimbursement environment.
This interest is likely to increase further as providers gain more experience in existing accountable care programs and begin to look for more options to increase their potential financial rewards.
By taking some elements from successful initiatives the past and adding in attractive benefit flexibilities and reduced administrative requirements, CMS hopes that GPDC will complement concurrent accountable care activities and that it may soon become a new framework for Medicare fee-for-service at large.
The DCEs that have secured licenses for this first iteration of the program have an unprecedented opportunity to establish themselves as true leaders in value-based care. With the right data-driven insights to help chart a path through this untested environment, DCEs can outperform their competition while measurably improving outcomes for Medicare beneficiaries in need.
To learn more about how andros can help you navigate the changing value-based care landscape visit https://andros.co/medicare-direct-contracting/